Innovation Through Claims Analysis – ECC March 2016
Setting the Scene
We were kindly invited to speak at the Eastern Claims Conference on March 14th about claim analytics and some of the work the Claim Lab is doing in this area. Below is a condensed version of the presentation and we have included some of the slides.

What is analytics?
The best and simplest definition I could find is: “information resulting from the systematic analysis of data”. What we do with data and how we use it is slightly more complicated.
Analytics’ are everywhere. Credit card companies, Amazon, weather forecasters and even the US postal office use analytics. We need to look at analytics as providing support for human judgement.
People have great memory, but can be biased by psychological aspects, and tend to overweight successes. Whereas, analytics are more objective, and take into consideration all historic information.
Building Analytical Models
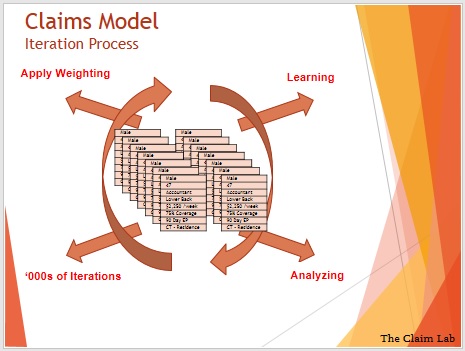
We’ve all studied the simplest version of analytics in high school when we learned linear regression. The Claim Lab’s model is quite a bit more complex, with over 30 variables accounted for, including date of disability, age, diagnosis, occupation etc. Typically, we go back 2 or 3 years in an insurer’s claim files, as beyond this the data is less effective.
Our model looks at thousands of claims and their outcomes. It learns what data items impact outcomes, applies weightings and analyses the differences between the claims. Once the model is complete, and has been tested, it can be used to assess new claims. When a new claim comes in, the model will look at the claim data and predict, in this case, the claims duration.
Claim Segmentation
Claim segmentation is a vital part of a more effective STD process, and analytics should be used to drive the segmentation rules. The Claim Lab produces Analytical Models to predict the duration of a STD claim, and from this you can start the segmentation process.
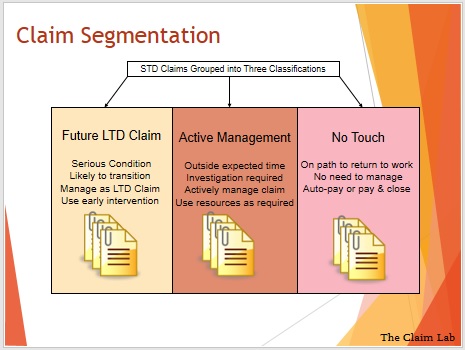
Here is an example of the STD claims being segmented into 3 buckets. The first segment is the ‘No Touch’ claims. These are the claims that are least serious and should be put through a “Pay-&-Close” or auto-adjudication process. It is this segment that saves the claims managers time so they can address the other segments.
So by contrast we also segment the most severe claims into the ‘Future LTD’ bucket, as you would expect these are the claims at high risk of transition to LTD. These claims need active management from the outset, and all the benefits of early intervention used.
The last segment shown here is the “Active Management Segment” which are claims that don’t meet the criteria for the other two groups but still need management.
We have seen companies taking variations on this approach. But the key fact is to use the ‘No Touch’ segment to save the claims managers time so the more serious claims can be managed effectively.
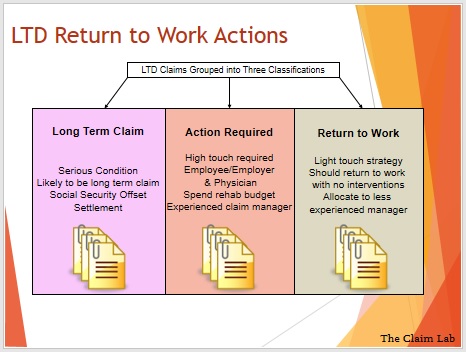
A similar technique is used for LTD claims, the buckets vary slightly as there is a wider variety of claim duration in LTD. We categorize claims as: ‘Return to Work’ ‘Action Required’ and ‘Long Term Claim’.
Intervention Analysis
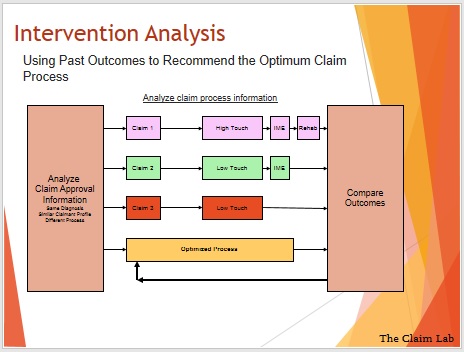
Intervention analysis looks at what happens to the claim post approval and helps you to understand where your dollars are having best effect.
So here we can see 3 claims with a similar profile being put through 3 different approaches. What we want to find out is which process is most effective, so the claim outcomes will be compared to see what is working and what is not working.
This will ensure your budget is used most effectively, and perhaps, more importantly, will design a claim management process that is more effective as a result.
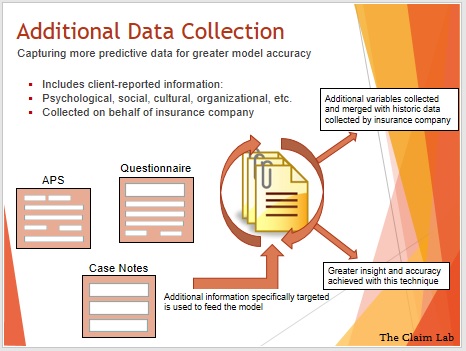
Additional Data Collection
One of the challenges of working with data, is the almost insatiable need for more. Claims systems were not designed with analytics in mind. They, therefore, do not always answer the questions we need, so we are constantly looking for ways to supplement our databases. This is traditionally done by looking at the claims notes, and questionnaires – but the format they are in means they are only of use to a claim manger – who needs to go through each one individually. This is time-consuming.
The Claim Lab has been working on changing the formats of these notes and responses, so that the data model can mine them for information to incorporate into its analysis. They cover aspects of wellbeing or diagnosis and are highly predictive. This is innovative research the Claim Lab is pioneering – we are currently recruiting companies to help us with a pilot.
Holistic Approach
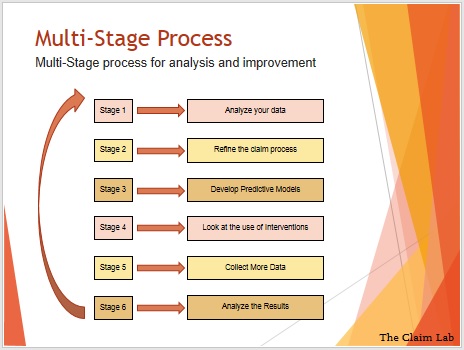
We recommend taking a holistic approach to implementing analytics in your claims operation.
Analytics is a process, it needs an objective, a plan, and commitment. We start by analyzing your data, to look at what is happening now. Then we look at the claims management process to understand why this is happening. At this point you can start building the analytical models, focused on a goal. From here we can look at interventions and how they are applied. This comes full circle again and we can add new data to improve the scope and accuracy of the models.
Innovation in Claims Management?
Analytics makes a profound difference to how we manage claims. Whilst it is still early days, it represents a chance for real innovation in the claims industry, so if you have not yet started incorporating it into your claims process, you better get a move on!
The Claim Lab – Email us at info@claimlab.org