Short Term Disability
“There is not enough time to manage claims properly”
“Either they get better or they go to LTD”
“We have so many claims that we cannot hope to be proactive”
These are things we hear constantly, and The Claim Lab has a better idea, let’s focus claim managers on the claims that need to be managed, and leave others that are highly likely to return to work.
Our STD Questionnaire will help a claim manager understand the individual behind the claim and identify barriers to return to work as early as possible and assign a “psychosocial risk factor” to the claim, using our AI driven risk models.
Risk Factors Include:
- Mental Health
- Motivation
- Workplace
- Domestic
- Financial
- Physical Capacity
Any claim where significant psychosocial risk factors are indicated could be at risk of transitioning to a long term disability claim, and should be monitored carefully.
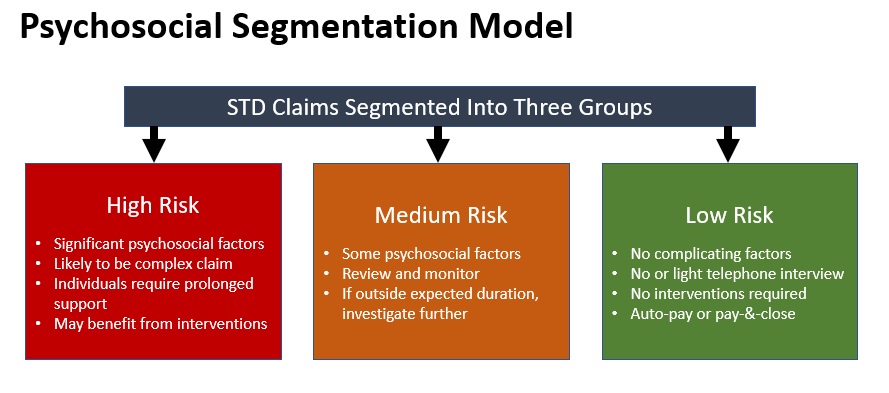
The diagram above shows the three classifications used to group STD claims:
High Risk – This classification indicates that the analytics suggest this claim has significant psychosocial issues that could delay return to work. This claim should be assigned to a more experienced case manager and a high-touch process used.
Medium Risk – This classification is for a claim where some psychosocial factors have been identified, and should be reviewed and monitored for any deviations from expected recovery path.
Low Risk – This is for a claim that has no psychosocial issues and needs a light-touch process, maybe a shortened or no telephone interview, freeing case managers to spend more time on more complex claims.
The Claim Lab – Email us at info@claimlab.org

