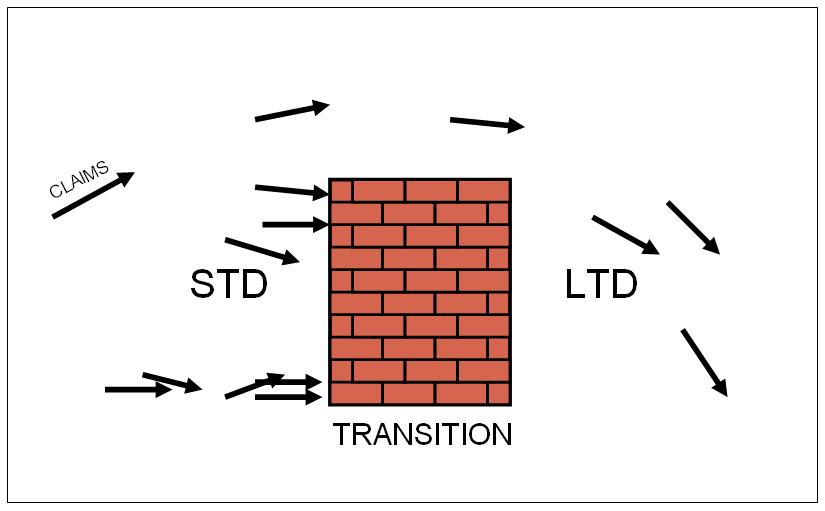
Reducing Transition Rates
Disability insurance carriers are under pressure to change STD processes. The product is just not profitable enough. Corporations buying group insurance are becoming more sophisticated, and using brokers to select their insurers.
The brokers are comparing carriers on the stuff that’s easy to measure, such as speed to making decisions, or time taken to get the first payment out.
Insurance carriers are managing their STD business to meet these standards to maintain competitiveness.
Meanwhile, they are perplexed by the numbers that suggest combined STD & LTD has worse experience than separated products.
Maybe the focus has shifted to the wrong end of the process. While everyone is jumping through the hoops set by brokers, who are trying to justify their existence, claims management, the real reason we are all here, is being neglected.
As we all know, claims are harder to manage effectively than the short-turnaround-times of the customer service world. There is a need for skilled claim managers in STD teams, and STD should not be treated as a training area for less experienced personnel.
It is possible for carriers to meet both of these objectives, but they need to embrace claim segmentation and they need to use innovative technology in the form of predictive models to drive the segmentation process.
Predictive models will enable the claims to be segmented more accurately, spotting those complex claims that don’t necessarily appear to be complex and processing the simple claims without claim manager intervention. This latter point will save claim manager’s time which can be used to focus on those complex claims.
By addressing the claims that could transition to LTD, your transition rate will reduce. In addition, STD claim managers should be given the tools used by the LTD claim managers and get the benefits of early intervention.
As for the analytics, this can be used to accurately profile the claims and predict what the future direction of the claim might be. Some of these profiles can reflect subtle differences in the information relating to a claimant, and can highlight the need for different handling.
With the help of analytics both objectives can be met, the demands of the customer service standards and managing claims and resources to reduce transition rates to LTD.
Innovation does not often occur in claims management, so this opportunity should be embraced.
The Claim Lab – Email us at info@claimlab.org